Preoperatively unrecognized difficult airway is responsible for a significant proportion of the morbidity and mortality caused by anaesthesia. Complications, such as hypoxic brain damage, cardiopulmonary arrest, surgical airway management and airway trauma, can have serious consequences for a patient’s health. The most serious complication of a preoperatively unrecognized airway is death, and research indicates that as many as 30% of deaths in anaesthesia are caused by failed intubation [1]. The American Society of Anesthesiologists (ASA) defines a difficult airway as a situation in which a standard-trained anesthesiologist encounters difficulty during mask ventilation, direct laryngoscopy, intubation, or combined [2].
The assessment of difficult airways in all surgical specialties is well studied in the literature, while research in ear, nose and throat (ENT) surgery is scant. In the case of other surgical specialties, difficult intubation occurs in 2.8–6.8%, while ENT surgery occurs in 15.8% of cases [3]. The patholo-gy includes the possible presence of orofacial trauma, tumors, and infections, as well as a positive history of previous surgery and/or radiotherapy in the head and neck area. These facts bring us to the question of the specific preoperative airway assessment methods that an anesthesiologist can rely on when it comes to ENT, especially to laryngeal surgery. Changes in the vocal cord and upper airway anatomy imply a greater possibility of a difficult airway. These patients often have varying degrees of hoarseness, stridor and upper airway obstruction. Laryngeal surgery also involves a shared airway with the possibility of compromising airway patency pre-, intra- or postoperatively [4–9].
ENT surgery, and especially surgery of the upper respiratory tract, implies the teamwork of an anesthesiologist and surgeon. Preoperative joint observation of the airway is of key importance for successful intubation [10]. Previous research did not explore the success of commonly used anesthesiological preoperative airway assessment methods in laryngeal surgery. We did not find any research dealing with the importance of cooperation between surgeons and anesthesiologists in ENT surgery. Our study aimed to find the most effective anesthesiological and surgical parameters and methods to predict difficult airways in laryngotracheal surgery preoperatively more accurately.
Given that there is no single score specific to ENT surgery among the many scores for assessing the difficulty of intubation, we believe that in the future, the parameters marked by this research will provide orientation for the formation of a new score for preoperative airway assessment specific to laryngeal surgery.
METHODS
This prospective pilot clinical study included 50 patients above 18, scheduled for microscopic laryngeal surgery at the Clinic for Otorhinolaryngo-logy, University Clinical Center in Niš, between June and September 2023. This study was approved by the Ethi-cal Committee of Medical School, University in Niš, Niš, Serbia and by the Ethical Committee of the University Clinical Center of Niš, Niš, Serbia. Criteria for inclusion in the study were: diagnosis of a lesion of the vocal folds, planned general endotracheal anaesthesia, age over 18 years and the absence of a tracheostomy. Exclusion criteria were: patients younger than 18 years, presence of a tracheo-stomy cannula, refusal of the patient to participate in our research, inability to understand and/or sign an informed consent form, and urgent surgical interventions. Each patient in the study was informed about our research and signed an informed consent form. Preoperatively, each patient underwent a regular surgical clinical examination, including flexible laryngoscopy. The surgeon preoperatively identified the possibility of difficult intubation based on the flexible laryngoscopy findings and previous experience.
Before the surgical intervention, an anesthesio-logist conducted an interview about the patient’s medical history and a detailed airway assessment. The attending anesthesiologist used a specially designed questionnaire to provide all the needed parameters and measurements. The patient’s gene-ral data, such as gender, date of birth, weight in kilograms (kg) and height in centimeters (cm), were entered. From these parameters, the body mass index (BMI) was calculated with the help of an online calculator that can be found at the following address: https://www.calculator.net/bmi-calculator.html. Data related to difficult intubation were entered, e.g. presence of stridor, general condition determined by the ASA score, loud snoring, feeling tired during usual activities, apnea during sleep and hypertension. The ASA score is determined by the official ASA classification used in everyday clinical practice.
Prediction of the difficult airway was performed first by observing the patient’s anatomical features, e.g., mandibular prognathism retrognathia and prominent incisors. Specific measurements and tests were conducted after the patient was seated. The examination began by ordering the patient to open his mouth as much as possible. Then, the distance between the upper and lower incisors (inter-incisor gap – IIG) was measured. The patient was then instructed to perform the modified Mallampati test (MMT) by pushing the tongue out of the oral cavity as much as possible while still in the previous position. The interpretation of both tests is given in Table 1.
TABLE 1
Interpretation of specific tests for prediction of difficult intubation
The mandibular protrusion test, known as subluxation (S-lux), was performed by instructing the patient to protrude the lower jaw in front of the upper jaw. The results were classified as follows: S-lux > 0 means that lower incisors can be protruded anterior to the upper incisors, and S-lux = 0 means that the lower incisors can be brought edge to edge with the upper incisors. S-lux < 0 means that the lower incisors cannot be brought edge to edge with the upper incisors. The interpretation of the results is given in Table 1.
For the second part of the measurement, the patient was instructed to perform maximal neck extension in a sitting position. Then, the thyromental distance or Patil’s test was measured together with the sternomental distance. The reclination test was performed in this position by instructing the patient to open his mouth and position the upper teeth horizontally about the surface. Then, the maximum extension of the neck was performed, and the angle of deflection of the upper teeth was determined. The interpretation of the reclination test is given in Table 1.
The length of the mandible, its anterior and posterior depth, neck circumference, and the acromion-acromion distance were measured.
All the patients were intubated using the direct laryngoscopy method, using a laryngoscope with a Macintosh blade, size 4. The intubation difficulty was determined by using the Intubation Difficulty Scale (IDS) immediately after the intubation was performed in the operating room. The data necessary for determining the IDS and their scoring are given in Table 2. By ”alternative technique” during intubation, we mean any modification of the intubation process that differs from the routine placement of the tube in the trachea. More precisely, it involves modification of the position and curvature of the tube during intubation, change of the patient’s position, use of a bougie, Magill forceps, and fiberoptic bronchoscope. After assessing the difficulty of intubation according to the results of the IDS, patients were divided into two groups: difficult intubation (DI) and standard intubation (NI).
TABLE 2
Calculation of the Intubation Difficulty Score (IDS) and its interpretation
All the results related to continuous variables are expressed as median ± SD. While there were different types of variables, the difference between the two groups was determined using the t-test for independent samples, the Mann-Whitney U test and the c2 test. A binary logistic regression model was performed to assess the interaction between variables. We used C statistics to evaluate the effectiveness of the combinations between two or more parameters. The area under the curve (AUC) was determined with sensitivity and specificity. A P-value below 0.05 was considered a statistically significant result. All results were statistically processed in the program SPSS 10.0 for Windows (SPSS Inc., Chicago, IL, USA).
RESULTS
We included 50 patients between 33 and 83 years of age (61.26 ± 10.87) in our study. The largest group of patients was between 51 and 60 years of age, comprising 18 (36%) patients. Nineteen (38%) patients were female and 31 (62%) were male. The body mass index (BMI) was 26.30 ± 5.51, which is categorized as overweight. The general characteristics of the patients are presented in Table 3, while the clinical characteristics that are essential for the prediction of difficult intubation are presented in Table 4.
TABLE 3
General characteristics of the patients
TABLE 4
Clinical characteristics of the patients
According to the IDS scale, 17 (34%) intubations were difficult. Patients in the DI group were more often of male gender (P = 0.033) and had apnea during sleep (P = 0.021). Flexible laryngoscopy provided insight into postoperative histopathological and site characteristics of biopsied tumors. As many as 20 (40%) showed malignant and 30 (60%) benign characteristics. There was no statistical significance regarding the histopathological characteristics and intubation difficulty, with P = 0.180. Details are presented in Table 5.
TABLE 5
Number and percentage of patients according to the histopathological and site characteristics of the tumor mass
Patients in the DI group had IIG below 4 cm, a higher class of reclination, a greater neck girth, and a higher class of MMT. Table 6 presents statistical details. Out of all the measured data and provided tests, the following showed statistical significance: IIG, reclination, neck girth, MMT, and flexible laryngoscopy. Flexible laryngoscopy showed the highest level of statistical significance, with P = 0.0001.
TABLE 6
Measurements and applied tests
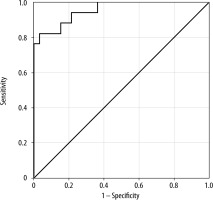
The statistically significant parameters were processed in C statistics, and the AUC curves are represented in Figure 1. Neck girth was the only scale variable that showed a new cut-off value of 40.70 cm, with a CI of 95%, sensitivity of 82.4% and specificity of 55.5%.
FIGURE 1
ROC curves of independent parameters: Gender AUC = 0.654 (95% CI; P = 0.033; 0.498–0.810), Apnea during sleep AUC = 0.660 (95% CI; P = 0.021; 0.490–0.831), IIG above 4 cm AUC = 0.617 (95% CI; P = 0.021; 0.443–0.791), Reclination AUC = 0.715 (95% CI; P = 0.037; 0.553–0.876), Mallampati test AUC = 0.679 (95% CI; P = 0.032; 0.513–0.845), Flexible laryngoscopy AUC = 0.749 (95% CI; P = 0.0001; 0.591–0.906), Neck girth AUC = 0.689 (95% CI; P = 0.021; 0.542–0.836)
Flexible laryngoscopy identified 13 (26%) patients as possible difficult intubations, compared to Cormack-Lehane classification results revealed during direct laryngoscopy. Flexible laryngoscopy correctly classified 39 (78%) patients, with c2 = 9.802, df = 1 and P = 0.002.
According to the results, flexible laryngoscopy was the best model for predicting difficult intubation. Therefore, we have estimated that this para-meter can be combined with other statistically significant parameters and measurements. A detailed review of all the statistical models is provided in Table 7. Among all the combinations of one parameter and flexible laryngoscopy, reclination had a greater impact on the statistical model than all the other parameters (Figure 2).
TABLE 7
Statistical models considering combination of flexible laryngoscopy with other statistically significant parameters
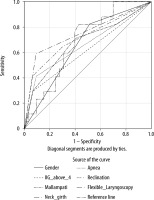
FIGURE 2
ROC curves showing the specificity and sensitivity of combination between flexible laryngoscopy and one of the statistically significant parameters: flexible laryngoscopy and gender AUC = 0.795 (95% CI: 0.656–0.935, P < 0.0001), flexible laryngoscopy and apnea during sleep AUC = 0.797 (95% CI: 0.651–0.935, P < 0.0001), flexible laryngoscopy and IIG above 4 cm AUC = 0.822 (95% CI: 0.686–0.957, P < 0.0001), flexible laryngoscopy and reclination AUC = 0.874 (95% CI: 0.770–0.979, P < 0.0001), flexible laryngoscopy and Mallampati test AUC = 0.830 (95% CI: 0.708–0.955, P < 0.0001), flexible laryngoscopy and neck girth AUC = 0.832 (95% CI: 0.700–0.959, P < 0.0001)
Then, we combined flexible laryngoscopy and reclination with other parameters, and there were no significant differences between statistical models, as shown in Table 8 and Figure 3.
TABLE 8
Statistical models considering combination of flexible laryngoscopy and reclination with other statistically significant parameters
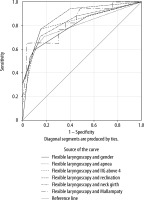
FIGURE 3
ROC curves showing the specificity and sensitivity of combination between flexible laryngoscopy and reclination with one of the statistically significant parameters: flexible laryngoscopy, reclination and gender AUC = 0.888 (95% CI: 0.796–0.979, P < 0.0001), flexible laryngoscopy, reclination and apnea during sleep AUC = 0.900 (95% CI: 0.800–1.000, P < 0.0001), flexible laryngoscopy, reclination and IIG above 4 cm AUC = 0.898 (95% CI: 0.797–0.998, P < 0.0001), flexible laryngoscopy, reclination and Mallampati test AUC = 0.895 (95% CI: 0.810–0.980, P < 0.0001), flexible laryngoscopy, reclination and neck girth AUC = 0.896 (95% CI: 0.805–0.987, P < 0.0001)
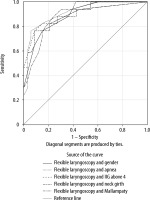
When we combined all the statistically significant parameters, the statistical model indicated that flexible laryngoscopy, reclination and neck girth contributed to the model to the greatest extent. This model showed statistical significance, with the values of c2 = 43.268, P < 0.0001, and an AUC of 0.955 (Figure 4).
DISCUSSION
Considering the specificity of ENT pathology, we expected that our results would differ from those obtained in studies that dealt with other surgical specialties. Namely, many parameters used in everyday anesthesiology practice, which were significant in other studies, did not show statistical significance in our research. Initially, discussing the discrepancy between the incidence of difficult intubations in the literature and our results is essential. Our study showed that difficult intubation was present in as many as 34% of examined patients. Also, according to the available literature, the incidence of difficult intubations in ENT surgery is 15.8%, more than two times lower than in our study. The mentioned incidence is present in the entire ENT pathology, while our patients were subjected exclusively to micro-laryngoscopy. It should be noted that some authors exclusively use the Cormack-Lehane score to determine difficult intubation, while in our study, a more extensive and accurate IDS score was used [3].
The undeniable limitation of our study is the small number of randomly selected patients, and the true incidence will be revealed only after the study is further expanded. Another limitation is that no developed classification would define the flexible laryngoscopy finding as potentially difficult or usual intubation in the field of laryngology. Therefore, we had to rely on the only classification available in practice, i.e. surgeon’s experience.
As regards the general data of the patients, statistical significance was found only in the case of gender, while other parameters failed to reach statistical significance. Several studies have found that the frequency of difficult intubation is higher in men, which is in correlation with our results [11–14]. Wong et al. [3] reported that a history of previous difficult intubations significantly predicts future difficult intubations. In our research, we did not obtain such data, probably because of the absence of such a data registry in our country. Patients are often not informed about a difficult airway during previous intubation.
Our study did not show statistical significance of the patient’s age in the summary or within the age groups. Oria et al. [15] found that age over 40 years was a predisposing factor for difficult intubation. Such results are explained in the literature by the fact that with age, specific anatomical changes lead to the appearance of a difficult airway [11, 16]. The lack of correlation with our results can be explained by the fact that the cause of difficult intubations lies in the pathology of the airway itself and the anatomical changes accompanying it. Age is not one of the main predictors of difficult intubation.
Considering the parameters used in determining BMI, none showed significance for predicting difficult airways. There are conflicting reports regarding BMI as a predicting parameter of difficult intubation [11, 17–20]. Moon et al. [11] found that even a group of morbidly obese patients did not have a higher frequency of difficult intubations but only a higher incidence of difficult mask ventilation. In an extensive study, Uribe et al. [17] found that BMI in men was a valuable parameter in predicting difficult intubation. However, only other surgical specialties were included. In their meta-analysis, Wang et al. [18] remained inconclusive regarding the accuracy of this parameter, which correlates with everyday clinical experiences.
Patients who undergo laryngeal surgery very often suffer from obstructive sleep apnea (OSA), which is a predisposing factor for difficult intubation. The parameters we examined that indicate the risk for an existing OSA, such as stridor, loud snoring, fatigue, high blood pressure, and endocrine comorbidities, did not show statistical significance. The only statistically significant parameter was the existence of OSA, which the patient already knows. OSA and increased neck circumference have been shown to be independent parameters for predicting a difficult airway in many studies [21–23]. Nerurkar et al. [24] reported that neck circumference has an impact on predicting difficult airways in microlaryngoscopy, which correlates with our results. The cut-off value found in their research was 37.5 cm, while in our study it was 40.70 cm. The fact is that neither their research nor ours included many patients, and a larger number of patients is necessary to determine a more precise cut-off. Riad et al. [25] stated that setting a cut-off value of 42 cm is essential. Further research is needed to set a more accurate cut-off value.
In our study, instead of measuring IIG and interpreting the results as a scale parameter, we used a cut-off value of 4 cm. This parameter was significant in our study and correlates with other studies [3, 26–28].
The MMP score is a good predictor [3, 11, 17, 29, 30]. However, studies have shown that it cannot be used as an isolated predictor [31]. Bergler et al. [32] concluded that MMP above 3 significantly predicts difficult intubation in oral surgery, with results that correlate with ours.
According to the AUC curves, reclination and flexible laryngoscopy are the only parameters that can be used as independent predictors of difficult intubation in laryngeal surgery. Alp et al. [33] confirmed that reclination can be used as an isolated predictor. Some studies have indicated that flexible laryngoscopy is a strong isolated predictor of difficult intubation [3, 34, 35]. Only the study by Budde et al. [36] showed a limited prediction and, according to the authors, a ”tendency towards statistical significance” in obese patients. No studies would combine flexible laryngoscopy as a strong predictor with anesthesiology parameters, which was one of our research goals.
The lack of statistical significance of many measurements and clinical assessments of difficult intubation in our study can be explained by the fact that all these parameters are significant but not sufficient for a precise evaluation of a difficult airway in laryngeal surgery. Even if they indicate the absence of a difficult airway, the anesthesiologist can face a possible challenge only after placing the laryngoscope and visualizing the airway. For this reason, in laryngotracheal surgery, the surgical assessment and joint discussion of the airway preoperatively are extremely important for timely equipment preparation and the surgical team’s surgical airway preparation. It is undoubtedly advisable to preoperatively look at as many parameters used in routine practice as possible. However, in the absence of time, it is necessary to look at specific parameters. Through our research, we have identified significant parameters that, after more extensive research, can be used to eventually develop a score for the preoperative assessment of the airway in laryngeal surgery.
The statistically significant parameters in our research are scores that allow greater head and neck extension and greater mandible manipulation when visualizing the glottis. With additional surgical observation, these parameters accurately assessed difficult airways in laryngeal surgery.
CONCLUSIONS
Difficult airway assessment could not be reliably defined using solely the anesthesiologic parameters. Flexible laryngoscopy must be included in the preoperative evaluation of ENT, especially laryngeal surgery. Further studies are needed to classify and make the flexible laryngoscopy findings more objective. We have identified parameters that can be used to develop a reliable and accurate score for preoperative difficult airway assessment in laryngeal surgery.